Although platelet-rich plasma (PRP) is often used to treat mild to moderate osteoarthritis (OA), this regenerative therapy remains controversial. Does PRP actually work for osteoarthritis pain?
Before exploring the controversy around PRP, let's clarify what this regenerative therapy involves. Platelets made by your body are known for their ability to form blood clots after injury. In addition to clotting proteins, platelets also carry dozens of types of growth factors. When you get a cut, bruise, or sprain, platelets stop the bleeding and then activate the healing process by releasing these growth factors and building block proteins.
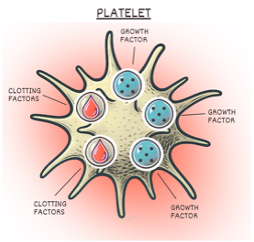
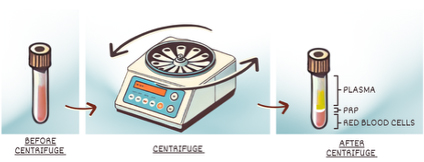
PRP was first used in the 1980s to treat difficult-to-heal wounds. It was found that if blood were anticoagulated to prevent its clotting and spun in a centrifuge, it would separate into three layers. Platelets would concentrate in the middle layer. When applied to stubborn wounds, this "platelet-rich plasma" accelerated healing. The growth factors in the platelets promoted the recruitment of rebuilding cells and the production of healthier tissues.
In the 1990s, the use of PRP expanded into other medical fields, including orthopedics and pain management. It was found that these concentrations of platelets and growth factors not only aided in wound healing but also provided benefits for those suffering from osteoarthritis. Several studies over the past decade have shown that PRP is more effective in the long term than other types of injections, such as hyaluronic acid. Meta-analyses (combined results from different studies) have also confirmed PRP's effectiveness in relieving osteoarthritis pain.
However, controversy arose in 2021 after two major studies on PRP for knee and ankle osteoarthritis were published. These studies found that PRP was no more effective than saline injections. These disappointing results greatly reduced interest in this regenerative treatment and led many physicians (and insurance companies) to see PRP as a waste of time and money.
How do we make sense of all this? Some studies showed significant pain relief for a year or longer, while others showed no effect at all. The answer becomes clear when we examine what the PRP in the research studies actually contained. It may seem obvious that platelet-rich plasma should be rich in platelets, but not all studies used plasma with high platelet counts. The two studies published in 2021 both used PRP with low platelet levels. Fewer platelets = fewer growth factors = no benefit. The importance of platelet count is further confirmed by other researchers, who have shown that PRP with high platelet counts improves pain and symptoms in individuals with osteoarthritis.
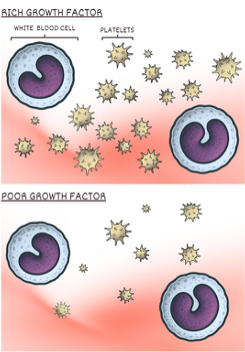
What does this mean for someone seeking non-surgical options for osteoarthritis pain? It means asking questions when talking to your doctor or healthcare provider. If you're considering the use of PRP, ask whether their process results in a high or low concentration of platelets. To maximize the chances of pain relief with PRP, a final dose of at least 5 billion platelets is necessary for larger joints such as the knee. Lower doses of platelets and their growth factors are unlikely to be effective in improving OA symptoms.
To be effective, platelet-rich plasma must be rich in platelets.