One of the most effective ways to stimulate the body's healing response for treating osteoarthritis (OA) and other chronic conditions is through exercise. The healing powers of exercise are increasingly acknowledged. What is less appreciated is that exercise resolves chronic inflammation by initially triggering acute inflammation. This apparent contradiction makes sense within the context of the healing immune cascade I describe in my book, which will be released in January 2026. I will summarize these ways in which exercise improves pain in osteoarthritis below.

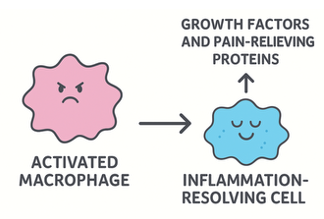
Exercise stimulates and harnesses an immune cell called the macrophage. Found throughout our bloodstream and tissues, macrophages perform various roles depending on their activation state. They are constantly moving and monitoring their environment. When activated by injury, they transform into large, aggressive cells capable of consuming invaders and even other immune cells. During this process, the activated macrophage releases multiple inflammatory proteins (cytokines such as TNF and IL-1), which cause pain and swelling during an injury, an osteoarthritis flare-up, or even a hard workout.
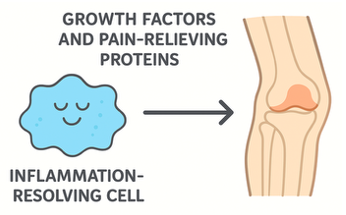
However, when the immune system functions properly, a remarkable transition occurs. The macrophage switches modes, transforming into an inflammation-resolving cell. This inflammation-resolver then starts producing growth factors and pain-relieving proteins, helping tissues to heal. Collagen production increases, cartilage becomes stronger, and pain decreases. The macrophage, activated by acute inflammation, becomes the architect of healing and repair.
Exercise is one of the most powerful tools to promote this healing macrophage and its growth factors. High-intensity exercise does it. So do lighter activities, such as walking. These benefits aren't just theoretical. Walking and similar exercises have been shown to slow the progression of cartilage damage in people with OA. Higher-impact sports such as tennis and running can also be beneficial for joints with OA when tailored to the individual's abilities. Strength training is another powerful tool. Building muscle enhances joint function and reduces pain in those with OA. Engaging in various types of exercise triggers immune-based healing processes.
Although anti-inflammatories like NSAIDs provide short-term relief from joint pain or muscle soreness, these medications can blunt the initial inflammatory response to exercise. By decreasing the number of activated macrophages, NSAIDs also slow the production of inflammation-resolving cells, limiting the benefits of exercise. Exercise is a powerful regenerative therapy that can improve joint health and repair damaged tissues. Whenever possible, it's best to avoid taking NSAIDs before your workout.
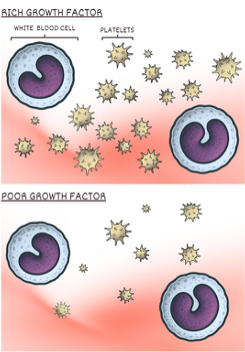
In the upcoming blog, I'll discuss a commonly used regenerative therapy that can also stimulate (in the proper dose) a healing immune response: platelet-rich plasma (PRP).